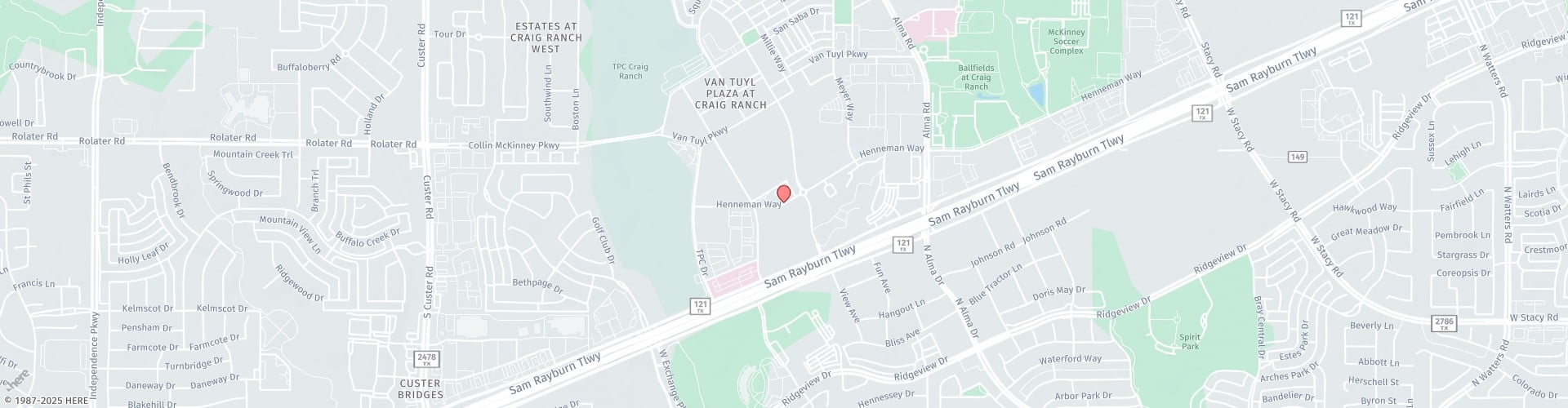
What Is Pelvic Pain?
Pelvic pain syndrome is a chronic condition that involves persistent pain in the lower abdominal and pelvic regions. Pelvic pain syndrome may be diagnosed when pelvic pain is chronic and has been present for more than 6 months. It can affect women both physically and emotionally, leading to sleep disturbances, anxiety, depression, and sexual dysfunction.

Pelvic pain can be a symptom of an underlying condition, or its cause may remain unknown. Living with pelvic pain syndrome is often difficult, and many women spend years trying to determine its cause. At Craig Ranch OB/GYN, we offer vast treatment options for your Pelvic pain. Our caring staff will do everything in our power to alleviate your discomfort.
How common is chronic pelvic pain?
Because pelvic pain can vary widely between patients, and because the causes can be traced or can be somewhat of a mystery, there aren’t great statistics on this condition. However, it’s estimated that between 15 and 20 percent of women between the ages of 18 and 50 may be affected. Many women deal with their chronic pelvic pain for over a year before they seek relief.
What Causes Pelvic Pain?
Chronic pain can be a mystery in many areas, and chronic pelvic is no different. Sometimes, there can be multiple factors causing the pain. Sometimes it’s a single source. Often, the pain is a result of one or more medical conditions. Unfortunately, in some women, the cause cannot be identified, and the goal is to help manage the pain.
These are some causes of pelvic pain syndrome:
- Endometriosis — In this condition, tissue from the lining of the uterus grows outside of the uterus. These deposits of tissue respond to the menstrual cycle, but because it’s happening outside the uterus the blood and tissue can’t exit the body through your vagina, and they remain in the abdomen. This can create painful cysts and fibrous bands of scar tissue.
- Musculoskeletal problems — Conditions that affect your bones, joints, and connective tissues, such as fibromyalgia, pelvic floor muscle tension, hernia, and others, can cause chronic pelvic pain.
- Chronic pelvic inflammatory disease — This can occur if a long-term infection causes scarring of your pelvic organs.
- Ovarian remnant — After a hysterectomy, a small piece of an ovary may be left inside and can develop painful cysts.
- Fibroids — Although they don’t usually cause acute pain, fibroid growths in the uterus can cause a feeling of heaviness in the lower abdomen.
- Irritable bowel syndrome — Symptoms associated with IBS, such as bloating, diarrhea, and constipation, can cause pelvic pain and ongoing pressure.
- Painful bladder syndrome — This condition involves recurring pain in the bladder and a frequent need to urinate. As the bladder fills, this can cause pelvic pain.
- Pelvic congestion syndrome — Although there is some disagreement here, some doctors believe the development of varicose-type veins around the uterus and ovaries can cause pelvic pain.
- Vulvodynia — Chronic vaginal pain and infections can lead to pelvic pain.
Could my pelvic pain be due to multiple causes?
There’s no reason your pelvic pain needs to have a single source. That’s what can make diagnosing the problem tricky. For instance, a woman with endometriosis can also develop uterine fibroids. The combination could increase her pelvic pain, especially during menstruation.
That’s why it’s a good idea to have ongoing pelvic pain checked out by the team at Craig Ranch OB/GYN. We can find out the cause or causes and help you deal with the pain.
What are the Symptoms of Pelvic Pain?
Patients with pelvic pain syndrome often experience the following:
- Constant or intermittent pelvic pain
- Severe cramping
- Muscle tenderness
- Pressure within the pelvic region
- Pain during intercourse
- Painful menstrual periods
- Fatigue
- Backache
- Pain during bowel movements or urination
- Pain when sitting for long periods of time
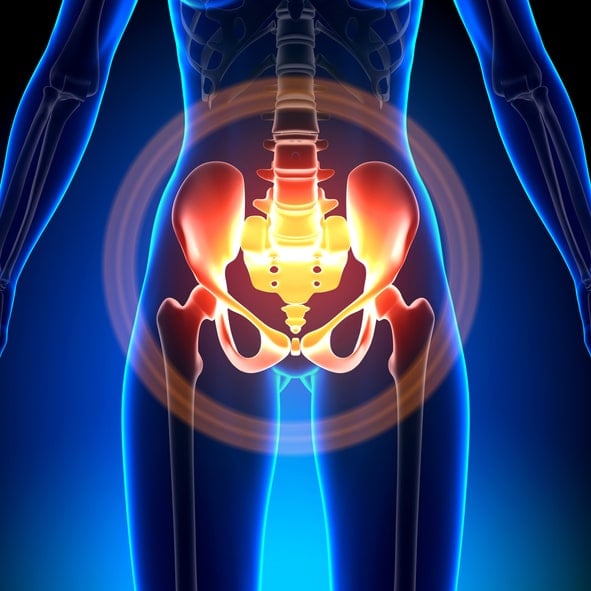
Pain in the pelvic muscles can lead to various problems and complications that primarily affect the bladder and the bowels. In some cases, the pain spreads to the back and legs. If these symptoms become severe or abundant, contact us to set up your consultation so we can begin treatment options for you.
How Do You Diagnosis Pelvic Pain Syndrome?
At Craig Ranch, Pelvic pain syndrome is diagnosed through a physical examination and a review of symptoms and the patient’s medical history. During the exam, the pelvis is checked for signs of infection or abnormal growth. Additional diagnostic tests may include the following:
- Laparoscopy
- Ultrasound
- Colonoscopy
- Cystoscopy
- CT scan
Treatment Options for Pelvic Pain:
Non-Surgical Pelvic Pain Treatment Options
Treatment of pelvic pain syndrome varies depending on its underlying cause. If an infection is a cause, antibiotics may be prescribed. If an underlying cause cannot be identified, treatment focuses on managing painful symptoms. Treatment can include the following:

- Pain medication
- Hormones
- Neurostimulation
- Antidepressants
Surgical Pelvic Pain Treatment
For some people, physical therapy that helps to develop healthier and stronger muscles can relieve symptoms. In severe cases, surgery may be recommended to treat underlying causes, such as endometriosis, or to remove scar tissue.
What can I do to manage my pelvic pain?
If your chronic pain is impacting your normal life, we need to see you at Craig Ranch. But short of that, there are things you can do to lessen your pain, or at least make it more tolerable.
- Over-the-counter pain relievers — Swelling can be causing your pain; ibuprofen or acetaminophen can relieve the inflammation and lessen the pain.
- Exercise — If you’re in pain, you may think exercise is the last thing you would want to do. But exercise increases blood flow, plus it can release endorphins, the body’s natural painkillers. Just 30 to 45 minutes of moderate exercise, 5 or 6 days a week, can help relieve your pain.
- Heat — A heating pad, warm compress, or a warm bath can help increase blood flow and decrease pain.
- Try some changes — If you’re overweight, try losing a few pounds, as this can relieve some pressure on your nerves. If you’re a smoker, stop. Nicotine inflames the nerves.
- Supplements — Sometimes pelvic pain can be due to low levels of key vitamins and minerals in the blood. Adding vitamin D, vitamin E, and magnesium supplements can help soothe chronic pelvic pain.
- Relax — Meditation, yoga, deep breathing exercises. Anything to reduce stress and tension and get your mind off your pain can be helpful.
When should I see a doctor for my pelvic pain?
Chronic pelvic pain is a pain in the area below your belly button and between your hips that lasts six months or longer. It can be hard to know when to see the team at Craig Ranch or another doctor for your pelvic pain. This varies by the patient, but it’s generally thought that if your pelvic pain begins to interfere with your daily life, or if your symptoms seem to be worsening, then it’s time to see a doctor.

Should I always see a doctor about pelvic pain?
Because there is such variation in pelvic pain in women, you wouldn’t say that any pelvic pain merits a visit to a doctor. However, if your pain becomes regular and chronic, it should be looked into.
Can Pelvic Pain Be a Symptom of an STD?
Tissue samples of the cervix or vagina may be taken to test for any signs of infection or sexually transmitted disease.
Patient Testimonials
Hands down, the best OBGYN facility I have ever been to. Amazing staff, from the receptionist, to the ultrasound tech, and don’t even get me started on nurses and doctors!!! I highly recommend this entire group!!! I promise, they will take care of you!
I couldn’t possibly love this group more!! They are so much more than doctors and medical staff. They care immensely for their patients and have gone above and beyond for me in the most caring ways. No other office compares!”
Schedule A Consultation
To schedule your consultation at our McKinney, TX office, call 214.544.6600. The providers at Craig Ranch OB/GYN are proud to serve patients in McKinney and the surrounding areas of Texas.